It's been a while, but I'm finally returning to my blog........
It's been just over 2 months since I last blogged so it's about time I stopped neglecting it. I enjoyed (and needed) the break from it I must admit but over the last couple of weeks I've been feeling the occasional urge to get back to the world of blogging.
Time to press the rewind button.......
My last post was all about the laser treatment (for Diabetic Retinopathy) that I had had on 31st August, which I had thought was going to be my last one for a while. Anyway, it turned out that I needed to have one more session so off I went back to the Eye Infirmary on 4th October for approx 1200 laser burns in my left eye and I was told that the next time I have to go in it will just be for a check up in 3 months time which was fantastic news. I'm really hoping that at the check up things will have stayed stable due to having better sugar levels since being on the pump!!! Fingers (and toes) crossed!!
So, what else has happened since my last post.....
We (me, Gareth and our 2 pooches, Poppy and Daisy) took part in one of Diabetes UK's Walk the Extra Mile events at the Lickey Hills Country Park on Sunday 12th September. I'd like to say a HUGE thank you to everyone who sponsored us. We managed to raise £248.00 in total which I was really pleased with and it's more than I have raised in the other years that I have done the walk. Next year I want to try and get up to at least £300.00 if possible. The weather was lovely and we had great fun, in fact I think the dogs enjoyed it way more than us!! I posted some photos on my Facebook page which you can see if you click on the link below:
http://www.facebook.com/permalink.php?story_fbid=1462007632199&id=1293715580#!/album.php?aid=280099&id=598130812
Now onto the most important part......the pump!!! I've now been 'attached' to Posy for 3 and a half months and I have to say its the best thing I ever did. Ok, so I've had some 'moments' (like yesterday for example) where I've wanted to rip the damn thing out and throw it against a wall but 99% of the time I'm very very happy with it and the results I've seen. When I started carb countng (in April) in preparation for going on the pump my HbA1c was 11.6 (horrendous I know), it had dropped to 8.8 in July and in September it had dropped a little bit more to 8.1 so although its not perfect yet, I'm certainly getting there!!!
I've had a few scary moments with the pump such as infusion sets popping out of their own accord and a "no delivery" alarm during the night which sent my blood sugar up to 33. I've had a few 'wobbles' about being constantly attached to a contraption forever, like when I'm in the shower and I see the pump sitting there on the side waiting for me to re-connect myself to it, but these moments soon pass and I just re-connect and carry on!!! I've also had a few instances where when changing the infusion set and priming the tubing the drops of insulin get onto the paper on top of the sticky bit and this then makes the sticky bit become unsticky - hope that makes sense!! It's quite frustrating when this happens, especially if I'm getting ready for work in a morning and I'm in a bit of a rush because it means starting again!!!! I use 'Mio' infusion sets so this might not happen with other types. However, one of my friends in the D.O.C. suggested a solution which I'm going to try tomorrow morning when I do a set change (hold the set upside down so the drops of insulin drip onto a tissue instead of down onto the sticky part - Thanks Angela, you're a star x x )
While I've been away from blogging we've had a bit of a stressful time at home which unfortunately had a bit of a negative affect on my dedication to the pump. Nothing drastic, but instead of being completely focussed on looking at patterns in my blood sugars and making adjustments according to those patterns, I have been tendng to just see the result and do what I needed to do at that point in time rather than building up a picture of whats going on with my levels at different times and whether certain foods make my levels rise etc. etc. I was comfort eating a fair bit too and just using the pump to compensate for any rubbishy foods I fancied eating!!! I did start to feel guilty about it all and had a bit of a confessing session when I last saw my DSN on 4th November. Funnily enough she said that when I started 'confessing' she thought I was going to say I didnt want the pump anymore so when she found out all it was was not paying quite as much attention to my levels as I had when I first got the pump, she was quite pleased!!! She also said that the way I started off being so focussed and dedicated to it was not a realistic way to carry on which made me feel a bit less guilty. The last thing I wanted her, or anyone else, to think was that I'd got my pump and was now just abusing it by eating tons of crappy foods and using it to compensate. I am very grateful for my pump and always will be but I do think that sometimes "life" takes over and other things get in the way and it really isnt realistic to focus on absolutely nothing but Diabetes every single second of the day. I hope this is making sense to at least a few Diabetics out there!!!! Anyway, I felt much better after "confessing" to Gill, my nurse, and she said I need to stop beating myself up so much because I have done brilliantly so far. We agreed that as my morning levels are still rising I need to do 3 overnight basal tests where I get up to test at 4am, 6am and 8am and then make adjustments to my basal rates according to the results of those 3 tests, over 3 days.
Since my last post I have met up with a lovely lady at work who also goes to Stafford Hospital and sees the same DSN (Gill) and consultant (Dr. Coates) as I do. We met up for lunch a few weeks ago which was great. I was really good to 'compare notes' and I must admit I did find it funny when we both sat down and immediately got our blood testing kits out!! (I've never been in that situation before so it was nice to not be the only person in the canteen doing a blood test!!!! Lol). She is on a different pump to me but it was good to see a different one in action and talk about the issues she has with hers.
I saw my consultant on 11th November and he said he is really pleased with my progress and that, if anything, my HbA1c has come down faster than they usually like to see. I had my bloods done again whilst I was there so I'm waiting for those results now. I dont expect it to have come down this time and if I'm honest I think it may even have gone up slightly but Dr. Coates said not to worry about it too much so I'm trying not to!!!! We also discussed, with my DSN and dietician, my next challenge which is to try and reduce the amount of carbs in my diet - easier said than done!!! Apparently my diet is pretty high in carbs and I need to have a re-think about my daily intake!!!!! Bad news as I LOVE my carbs!!!!! They said that they are pretty surprised that I haven't put a lot more weight on, especially as I apparently eat such a lot of carbs, because usually with every 1% drop in HbA1c you can expect to put on around 4 pounds in weight which would mean I should have put on approximately 12 pounds but I have only put on 2 pounds (so far). They mentioned to me about maybe starting to take Metformin in the future which is a tablet that can help with insulin resistance, appetite control and weight loss. I'm not ready for that yet though as I want to make sure I've tried everything I can with the pump first before starting to take yet another tablet - I'm sure I would rattle if I jumped up and down!!!
Well, I think thats quite enough for one day, its great to be back but I need to ease myself back into it gently I think!!!! Lol :o)
Tuesday, 23 November 2010
Friday, 17 September 2010
Eye hate to say eye told you so......
I've been neglecting my poor blog lately and it's been almost a month since my last post so I'm going to go back in time a bit to 31st August and to my last eye infirmary appointment.....
31st August 2010
Back at the Eye Infirmary for what I thought was going to be my last laser treatment for a while.....
As you will know if you read my post on my last visit to the Eye Infirmary, it didn't go too well and I wasn't happy with the doctor that I saw as she refused to give me the anaesthetic injection that I always usually have in my eye before the laser, which meant that I was in a fair amount of pain. I mentioned in my post about my last appointment that I got the impression she was in a rush and couldn't really be bothered to do it and she just wanted to get me in and out as fast as possible.
As I said, I was expecting this appointment to be on my left eye as I was under the impression that my right eye had been finished for the time being at my previous appointment.....Wrong!!!
When the nurse did the pre-laser checks I made sure that I was definitely down to have the anaesthetic this time and she went and confirmed with the doctor that this was the case. The doctor I had this time was a million times nicer than the one I had last time. He really put me at ease and said he could see from my notes that I should have the anaesthetic injection because of the amount of laser I have had in the past (the more you have the more painful it becomes because of the scar tissue that has formed).
Then it was time to have the anaesthetic injection....aaaaggghhh!!! Although having it is great in terms of making the laser treatment itself bearable it's not a nice procedure as it involves cutting the eyeball and injecting the anaesthetic into it....obviously I've never seen how it looks when they do it but Gareth has been there when they have done it and having a strong stomach he was able to watch what they do and then tell me all the gory details afterwards!!!!!
They put anaesthetic drops in first to numb your eyeball so you can't feel the cut/injection and all you can feel is an intense pressure pressing down on your eyeball. The doctor actually had to make the incision twice this time because he said the anaesthetic fluid wasn't going in properly....I felt like saying "too much information thanks" but was feeling too sick at the thought of it all to speak at that point!!!! The worst part was sitting up afterwards and feeling like I had tears rolling down my cheeks so I wiped my face and when I looked at my hand it was actually blood, not tears!!!!! Yuk!!! Having the injection also means that recovering from the laser takes longer and your eye is left in a bit of a mess for a few days.
Then the doctor said "Ok, so I'm lasering your right eye today....", I said "Errrr, no I had my right eye done last time so it should be my left today". He then told me that last time the doctor had only done 200 laser burns which in his words was "peanuts" and "a waste of time". As you can imagine I was not impressed as it now means I have to go back and have my left eye done on another day which means having more time out of work and more discomfort all because that doctor couldn't be bothered to do her job properly last time!!!!
Anyway, on with the show and on with the lasering. This time even with the anaesthetic, it didn't numb all of the pain in certain parts of my eye. In the end he told me had done 1359 laser burns which really put into perspective how few burns the previous doctor had done and that it really had been a waste of time!!!!
Off I went with a patch and a tube of cream to put in three times a day for a few days. For a few hours it's fine because the anaesthetic is still working and you can't feel anything but once it starts to wear off the whole side of my face felt like I had done a few rounds with Mike Tyson!!!!
As you can see from the picture my eye didn't look too pretty afterwards and the anaesthetic means you get double vision as it wears off, it's bloody painful, gave me blurred vision for a few days and the redness took twice as long as it has in the past to disappear. All in all it's not a nice procedure but it has to be done and I'm just grateful that there is a treatment available to save my sight. Now I've got my pump I'm assured that I will need to have treatment less frequently as having more stable sugar levels will help to prevent further bleeds, so that's brilliant news :o)
Having Retinopathy diagnosed a few years ago was terrifying and it was hard not to automatically think the worst and imagine going blind in the near future but luckily the laser can prevent that from happening, so given a choice between losing my sight and having a few days of soreness and redness every so often I know what I will choose every single time!!!
I'm hoping I never have that particular doctor again for laser treatment but if I did I wouldn't be able to resist saying: "Eye hate to say eye told you so doctor, but you really should have given me the anaesthetic shouldn't you" ;o)
Tuesday, 24 August 2010
Two weeks in.....
It's now been just over 2 weeks since I got my insulin pump. It's been......challenging, exciting and also, I have to say, pretty tiring!!!
I have been able to be in constant contact with my DSN (Diabetes Specialist Nurse), Gill, which has been brilliant and really reassuring to know that theres an expert on the end of the phone who can help with problems and panics. I have been texting Gill each morning (at her request) to let her know what my blood sugar levels have been over night and also to make suggestions as to what adjustments I think I should make.
I have been testing my sugars between 6 and 10 times per day which is much much more than I ever did in the past but it's necessary so that you can see exactly what your blood sugars are doing according to your doses and according to how much and what food you have eaten. It is important to keep accurate and detailed records of all of your blood sugar test results, exercise, what you eat and other things such as being ill so that your basal rates and bolus doses can be altered accurately. With accurate records you can then see patterns start to emerge at certain times of the day and/or when you eat certain things so you can then make the necessary adjustments.
Frequent testing is also essential because an insulin pump only delivers fast acting insulin so you don't have any long acting insulin in your system as a back up, therefore, if insulin delivery gets interrupted whilst on an insulin pump your blood sugars can go dangerously high in a pretty short amount of time so you need to know what is going on so you can treat high blood sugar levels quickly.
To test whether my overnight basal rates are correct I have been getting up at midnight and 3.00 a.m. to test my blood sugars - hence being so tired at the moment. My levels have still been fairly high in the mornings so that means I probably need more insulin overnight.
I have been having a lot more hypos since starting on my pump. Hypos were virtually non-existent for me in the past but now I'm having at least one a day which isn't fun. The lows seem to be mid afternoon and a couple of hours after my evening meal so now we need to work out whether it's my basal rates that are too high at those times of the day or whether it's my insulin to carbs ratio before lunch and before dinner that needs to be changed.
I've had a few panics and dramas like when I managed to put the infusion set in a stupid place (where a roll of fat creases over when I sit down - Yes, I know that's not a very attractive image I've just conjured up for you - Sorry!!) and it was really quite painful. I persevered with it but then at work I bent over to pick something up and the infusion set popped right out of my stomach...... Aaaaaaggghhh, I almost had a heart attack and went into total panic!!! Then I managed to replace the infusion set without filling the tubing first because I was in a panic and wasn't concentrating on what I was doing!!
Changing the infusion set and reservoir has been fairly easy so far (apart from the daft mistakes I mentioned above). At the moment I'm following the user guide to the letter each time I do it and it's taking me about 15 to 20 minutes but I'm told that I'll soon have it down to about 5 minutes!!!
Not doing injections is fantastic and has also been quite strange. For the 1st few days it was a struggle to remember not to jab myself and it felt like something was missing!!! But it hasn't taken me long to get used to it and appreciate the fact that not injecting after 19 years is absolutely amazing and I never want to go back!!!!!
I've enjoyed showing off my pump and explaining to people all about it and how it works. A couple of people at work have asked me "Whats that in your pocket?" when they have seen the tubing and I've been really happy to show them and tell them all about it. I will carry on rambling on about my new bit of kit for as long as people are interested and want to listen!!!
So far, going from injections to an insulin pump has felt a bit like a full time job at times, trying to keep up with what's going on with my sugars and what I need to do with the pump, counting carbs and then remembering what to do when I need to change the infusion set and insulin reservoir and I've felt like my brains been in meltdown but I know it will be all worth it.
One small thing I don't like about being on an insulin pump is that I now have to carry around a load of extra 'D' related stuff!!! Insulin pump kit = Glucose tablets, blood sugar testing kit and record diary, pen, carb counting books, blood ketone monitoring kit and/or urine ketone monitoring strips, spare insulin pen (for just in case there are problems with the pump), infusion set, reservoir, vial of insulin, antibacterial hand gel, spare AAA batteries, Glucagon injection (for use during a hypo when you are unable to swallow glucose tablets or glucogel) and snacks (such as cereal bars)......I think that's everything!! Obviously it's only a minor irritation but it certainly requires a huuuuuuge bag to carry it all around in....perfect excuse to buy a nice new bag if you ask me!!!! :o)
I'd like to say a big thank you to everyone who has asked how I'm getting on, offered tips and advice and who has just been there to support me during the last 2 weeks. I have to say that the people I have met in the Diabetic Online Community have helped me massively with the transition from injections to insulin pump and it certainly makes things a lot easier when you know there are people you can talk to online and ask what you may think are daft questions. There are always people willing to offer advice and help which is invaluable!!! THANK YOU!!!
Also, a huge thank you to my other half, Gareth, who has been fantastic. He has been there every step of the way for me, been to every appointment with me, put up with my moods and frustrations and he continues to help me with getting to grips with the pump.....I couldn't have asked for a more supportive partner!!! THANK YOU!!!! x x x
Last but certainly not least, I want to thank my Mom for being there for me from the very start of my Diabetes journey.....it's not always been easy, especially the teenage years when I refused to fully acknowledge my Diabetes. It's only now that I realise how awful this must have been for my Mom and what a nightmare it must have been for her when nothing she did or said would get through to me. I hope now that I have taken hold of this condition and accepted responsibility for my Diabetes I can make her proud of me. Love you Mom and thank you so so much for everything!! x x x
So to conclude, 2 weeks in, do I prefer the pump to injections??? Of course I do!!!
Tuesday, 17 August 2010
New beginnings on the Insulin Pump
So, here goes......this is my first blog as an insulin pumper.....do I feel different?? Well, apart from sitting at the laptop now wearing my new permanent attachment, not really, but it's certainly been an interesting first few days!!!
MONDAY 9TH AUGUST 2010 - Awake bright and early due to happiness, excitement, fear, nervousness and anxiety all rolled into one. Got up and did my last ever injection which I have to say was a pretty surreal and momentous occasion!!! It was a really strange feeling to be doing my last injection after just over nineteen years of doing them day in day out. Mixed emotions really as in a weird way, although they can be a pain to do and are sometimes painful (especially lately) the injections feel "safe" and reliable and you know for sure that the insulin has gone into your system whereas with a pump you are reliant on a machine to do the work for you and as we all know, machines can malfunction from time to time. (On the pump there might still be the odd occasion when I will need to inject, if the pump goes wrong for some reason, but this was my last "official" injection).
It felt a bit like I was standing on the edge of a cliff ready to jump off into the unknown because I still felt like there was SO much I didn't know about using an insulin pump. Obviously the day at the hospital was going to clear all of that up but before we set off I felt more than a little overwhelmed by everything I was still to learn and my new way of life.
My DSN, Gill, has been and continues to be fantastic and she made me feel at ease right from start of the day. First of all we went through all the bits and pieces in the box and had a look at all the supplies and things that go with a new insulin pump. Next we went through the menus on the pump. Gareth got to do all of the same steps along with me because Gill let him use her spare demo pump so he could see exactly how to use a pump too which was really useful.
We then looked at basal rates and how to set them. The insulin pump mimics a normally functioning pancreas by delivering insulin continuously over 24 hour periods, this is your basal rate and accounts for around one half of your body's total daily insulin requirements. Basal insulin is delivered at a rate of so many units per hour to cover your body's insulin requirements between meals and at night. Basal rates can be reduced when you are going to do some exercise so that your blood sugar does not go too low and can be increased when you are ill to stop your sugar levels going too high. The Medtronic Minimed Paradigm Veo allows you to set multiple basal rates for different times during a 24 hour period. Gill had calculated that I would start on one unit per hour. This would just be a starting point and it is likely that I will need to adjust them at certain times of the day until I get the dose I need to ensure that my blood sugar levels stay on target.
Next we looked at how to give bolus doses. Bolus insulin doses are given on demand when you eat or to correct a high blood sugar level. You work out the bolus dose you need according to the amount of carbohydrates you are going to eat. My current insulin to carbohydrate ratio is 2 units to 10 grams of carbs so for example if I was going to eat 20 grams of carbs I would need to give myself 4 units of insulin. Bolus doses are also used to correct a high blood sugar. To work out how much insulin you need to take to bring your blood sugar back down to your target level you need to know your insulin sensitivity factor. Gill had worked this out for me. To bring my blood sugar down by 1.1 mmol I need to take 1 unit of insulin.
As you can see there are a fair few calculations involved in this insulin pump lark!!! Once you tell the pump your target blood sugar range, your insulin to carb ratio and your sensitivity factor then it can work everything out for you but at first Gill wanted me to work it all out on paper so that I fully understood the calculations and what they mean. Once I had mastered this we could start to use a function called the Bolus Wizard which, like I said, works everything out for you. We did a few practice calculations on paper then it was time to learn how to fill the reservoir with insulin and connect the infusion set.
There are several bits of kit you need to have in order to get the pump ready to connect to your body.....a vial of insulin, a reservoir and an infusion set. The reservoir connects to the top of the vial of insulin and you draw back the plunger slowly to draw up the insulin into the reservoir. You have to do this really slowly so that you don't get bubbles in the insulin. If there are some bubbles you need to tap the reservoir to get rid of them.
Once you have made sure that the pump is fully rewound you insert the reservoir into the pump and you need to fill the tubing with insulin. This is all done by following the instructions on the pump screen. Apologies if this is hard to follow, its quite hard to explain all of the steps involved without this being like a copy of War and Peace, especially as I can't actually show you what I'm typing about!!!!
You are then ready to connect the infusion set to your body. The infusion sets I'm using are called Mio's. It is important to make sure that the insertion site is clean and that you rotate the site you are using each time you change the infusion set, which should be every 2 to 3 days.
The big moment........I was about to get connected!!!! I chose a site and fired the cannula into my stomach and 'hey presto', I was connected. (Firing the cannula into my stomach sounds a bit drastic but I couldn't think of any other way to describe it - again, it's difficult to describe something when you can't see what I'm talking about). Gill shook my hand and said "Congratulations, you are now an insulin pumper".....WOW!!! I could hardly believe it was happening and I didn't know quite what to say!!!!
Then I got to use my new blood glucose testing meter which tells the pump via bluetooth what your test results are....it's all very clever you know!!! :o
I was then let loose on my own and we went to have lunch and I had to work out the carbs in my meal and work out how much insulin I needed. Bit daunting but with the help of the calculator on my phone we managed to work it all out and away I went......I had given myself my first bolus dose on my pump!!!
The afternoon was spent discussing what to do if I had either high or low blood sugars and when to go back to injecting if there was a problem with the pump.
I was due to go back to the hospital on Wednesday afternoon when I would learn how to use the Bolus Wizard and would do my first set change. Gill wanted me to contact her at 6.00pm and 10.00pm to let her know how things were going which was a great reassurance for me as I felt like I had some back up if anything did go wrong.
My blood sugars over the next 24 hours were a bit up and down but that was to be expected until things settled down. It had also been a pretty stressful/emotional day so that can sometimes affect sugar levels too.
Gill let Gareth take home her spare demo pump so we could both have a look through the menus again and familiarise ourselves with them without actually doing anything on my "live" pump. Once we got home I persuaded Gareth to get connected aswell so he could see what it was like for me. I realise its not possible but I think it would be great if all hospitals could allow partners/spouses of Diabetics and parents of children with Diabetes to do this so they can get a real insight into what its like to wear one and also so that they have as much knowledge as possible about the pump and how it works.
All in all, a very successful day and the start of my new way of life. I know its not going to happen overnight and that there is some hard work to go into getting doses right to ensure I hit my target blood sugars and bring my HbA1c down to where I want it to be but I am really positive about the future and I am looking forward to seeing the great results and improved quality of life I know my new insulin pump can bring.
Oh, and one more thing.....I have decided to name my new pump "Posy" - so here's to a long and happy relationship with my new best friend.....Posy Pump!!!! :o)
MONDAY 9TH AUGUST 2010 - Awake bright and early due to happiness, excitement, fear, nervousness and anxiety all rolled into one. Got up and did my last ever injection which I have to say was a pretty surreal and momentous occasion!!! It was a really strange feeling to be doing my last injection after just over nineteen years of doing them day in day out. Mixed emotions really as in a weird way, although they can be a pain to do and are sometimes painful (especially lately) the injections feel "safe" and reliable and you know for sure that the insulin has gone into your system whereas with a pump you are reliant on a machine to do the work for you and as we all know, machines can malfunction from time to time. (On the pump there might still be the odd occasion when I will need to inject, if the pump goes wrong for some reason, but this was my last "official" injection).
It felt a bit like I was standing on the edge of a cliff ready to jump off into the unknown because I still felt like there was SO much I didn't know about using an insulin pump. Obviously the day at the hospital was going to clear all of that up but before we set off I felt more than a little overwhelmed by everything I was still to learn and my new way of life.
My DSN, Gill, has been and continues to be fantastic and she made me feel at ease right from start of the day. First of all we went through all the bits and pieces in the box and had a look at all the supplies and things that go with a new insulin pump. Next we went through the menus on the pump. Gareth got to do all of the same steps along with me because Gill let him use her spare demo pump so he could see exactly how to use a pump too which was really useful.
We then looked at basal rates and how to set them. The insulin pump mimics a normally functioning pancreas by delivering insulin continuously over 24 hour periods, this is your basal rate and accounts for around one half of your body's total daily insulin requirements. Basal insulin is delivered at a rate of so many units per hour to cover your body's insulin requirements between meals and at night. Basal rates can be reduced when you are going to do some exercise so that your blood sugar does not go too low and can be increased when you are ill to stop your sugar levels going too high. The Medtronic Minimed Paradigm Veo allows you to set multiple basal rates for different times during a 24 hour period. Gill had calculated that I would start on one unit per hour. This would just be a starting point and it is likely that I will need to adjust them at certain times of the day until I get the dose I need to ensure that my blood sugar levels stay on target.
Next we looked at how to give bolus doses. Bolus insulin doses are given on demand when you eat or to correct a high blood sugar level. You work out the bolus dose you need according to the amount of carbohydrates you are going to eat. My current insulin to carbohydrate ratio is 2 units to 10 grams of carbs so for example if I was going to eat 20 grams of carbs I would need to give myself 4 units of insulin. Bolus doses are also used to correct a high blood sugar. To work out how much insulin you need to take to bring your blood sugar back down to your target level you need to know your insulin sensitivity factor. Gill had worked this out for me. To bring my blood sugar down by 1.1 mmol I need to take 1 unit of insulin.
As you can see there are a fair few calculations involved in this insulin pump lark!!! Once you tell the pump your target blood sugar range, your insulin to carb ratio and your sensitivity factor then it can work everything out for you but at first Gill wanted me to work it all out on paper so that I fully understood the calculations and what they mean. Once I had mastered this we could start to use a function called the Bolus Wizard which, like I said, works everything out for you. We did a few practice calculations on paper then it was time to learn how to fill the reservoir with insulin and connect the infusion set.
There are several bits of kit you need to have in order to get the pump ready to connect to your body.....a vial of insulin, a reservoir and an infusion set. The reservoir connects to the top of the vial of insulin and you draw back the plunger slowly to draw up the insulin into the reservoir. You have to do this really slowly so that you don't get bubbles in the insulin. If there are some bubbles you need to tap the reservoir to get rid of them.
Once you have made sure that the pump is fully rewound you insert the reservoir into the pump and you need to fill the tubing with insulin. This is all done by following the instructions on the pump screen. Apologies if this is hard to follow, its quite hard to explain all of the steps involved without this being like a copy of War and Peace, especially as I can't actually show you what I'm typing about!!!!
You are then ready to connect the infusion set to your body. The infusion sets I'm using are called Mio's. It is important to make sure that the insertion site is clean and that you rotate the site you are using each time you change the infusion set, which should be every 2 to 3 days.
The big moment........I was about to get connected!!!! I chose a site and fired the cannula into my stomach and 'hey presto', I was connected. (Firing the cannula into my stomach sounds a bit drastic but I couldn't think of any other way to describe it - again, it's difficult to describe something when you can't see what I'm talking about). Gill shook my hand and said "Congratulations, you are now an insulin pumper".....WOW!!! I could hardly believe it was happening and I didn't know quite what to say!!!!
Then I got to use my new blood glucose testing meter which tells the pump via bluetooth what your test results are....it's all very clever you know!!! :o
I was then let loose on my own and we went to have lunch and I had to work out the carbs in my meal and work out how much insulin I needed. Bit daunting but with the help of the calculator on my phone we managed to work it all out and away I went......I had given myself my first bolus dose on my pump!!!
The afternoon was spent discussing what to do if I had either high or low blood sugars and when to go back to injecting if there was a problem with the pump.
I was due to go back to the hospital on Wednesday afternoon when I would learn how to use the Bolus Wizard and would do my first set change. Gill wanted me to contact her at 6.00pm and 10.00pm to let her know how things were going which was a great reassurance for me as I felt like I had some back up if anything did go wrong.
My blood sugars over the next 24 hours were a bit up and down but that was to be expected until things settled down. It had also been a pretty stressful/emotional day so that can sometimes affect sugar levels too.
Gill let Gareth take home her spare demo pump so we could both have a look through the menus again and familiarise ourselves with them without actually doing anything on my "live" pump. Once we got home I persuaded Gareth to get connected aswell so he could see what it was like for me. I realise its not possible but I think it would be great if all hospitals could allow partners/spouses of Diabetics and parents of children with Diabetes to do this so they can get a real insight into what its like to wear one and also so that they have as much knowledge as possible about the pump and how it works.
All in all, a very successful day and the start of my new way of life. I know its not going to happen overnight and that there is some hard work to go into getting doses right to ensure I hit my target blood sugars and bring my HbA1c down to where I want it to be but I am really positive about the future and I am looking forward to seeing the great results and improved quality of life I know my new insulin pump can bring.
Oh, and one more thing.....I have decided to name my new pump "Posy" - so here's to a long and happy relationship with my new best friend.....Posy Pump!!!! :o)
Friday, 6 August 2010
Ten becomes Nine!!!!
I have just worked out that I have only TEN injections left to do before I go onto my insulin pump on Monday!!
After 19 years of either 2 or 4 injections per day this is an amazing realisation. Let's say I did approximately 10 years at 2 per day and 9 years at 4 per day, that's 20,548 injections since diagnosis so to think I now only have TEN left to do is mind boggling and very very exciting!!!!!!
(Going onto the pump does not mean that I will never have to inject ever again, as there may be problems with the pump such as the tubing becoming clogged and I will have to keep spare injections for these instances)
Over the years when people have asked how I feel about injecting I have always said it doesn't really bother me that much, it's just something you get used to and at the end of the day it has to be done whether you like it or not.
Lately though it has started to become really quite painful every time I inject and I've started to actually "think" about it before I put the needle in whereas I used to just stick it straight in (for want of a better phrase) without even thinking about it. So now I think I would say that yes, injecting does bother me and for the first time in a long time it feels like a big deal to have to do it 4 times a day. That's why the thought of just TEN more is so fantastic.
Anyway, I'm off to do my Lantus, so that makes it just NINE more injections to do!!!!! :o)
After 19 years of either 2 or 4 injections per day this is an amazing realisation. Let's say I did approximately 10 years at 2 per day and 9 years at 4 per day, that's 20,548 injections since diagnosis so to think I now only have TEN left to do is mind boggling and very very exciting!!!!!!
(Going onto the pump does not mean that I will never have to inject ever again, as there may be problems with the pump such as the tubing becoming clogged and I will have to keep spare injections for these instances)
Over the years when people have asked how I feel about injecting I have always said it doesn't really bother me that much, it's just something you get used to and at the end of the day it has to be done whether you like it or not.
Lately though it has started to become really quite painful every time I inject and I've started to actually "think" about it before I put the needle in whereas I used to just stick it straight in (for want of a better phrase) without even thinking about it. So now I think I would say that yes, injecting does bother me and for the first time in a long time it feels like a big deal to have to do it 4 times a day. That's why the thought of just TEN more is so fantastic.
Anyway, I'm off to do my Lantus, so that makes it just NINE more injections to do!!!!! :o)
Wednesday, 4 August 2010
Countdown to Connection
My insulin pump start date is getting closer and closer.....my overwhelming emotions in relation to this are obviously elation and excitement but I have to admit it......I'm also slightly nervous and scared.
I'm sure some people won't understand how I can be feeling anything but excitement about getting my pump, especially people who have had or are having a fight on their hands to get one. I certainly don't want to annoy anyone by sounding ungrateful because that is not the case at all, I am extremely grateful for the opportunity I have been given and always will be.
It's hard to explain my feelings about Monday.....
I guess the word would be "apprehension". There are a few things I feel a bit nervous about, one being the fact that I will be more or less permanently attached to something for the rest of my life....ok, so I got on fine with it during my 3 day trial at the weekend and I do know that you can disconnect for short periods of time, but I do feel a bit freaked out by the "alien" element of it all. I have done a bit of reading on accepting being attached to the pump in my new "bible" (Pumping Insulin by John Walsh and Ruth Roberts). It mentions that some people may feel embarassed or self conscious about wearing a pump. I have to say that I am not concerned about that at all, in fact I am quite looking forward to telling people about it and explaining what it is and how it works, as it is certainly nothing to be ashamed of and I think the more people that know what it is and understand something about how it works the better. It's not how it looks to other people that concerns me, I think for me it's the "attachment" element of it which is quite hard to put into words. If anyone else had similar thoughts before starting on their pump please let me know.....(then again it might just be me!!! Lol)
Again, I do want to make it really clear that overall I am VERY happy about getting my pump and these negatives I'm talking about today are only small niggles, not major concerns!!!! I think it would be difficult to do something so life changing without feeling some sort of nervousness or anxiety.
I have been doing injections for 19 years now (first with a syringe and a glass vial of insulin that you had to draw up into the syringe yourself then with pens with cartridges that you changed and then finally with disposable, pre-filled pens) so I think I am going to find it really strange at first when I no longer have to reach for the insulin pen at set times of the day and for a while I might have to get Gareth to hide my pens so I don't inject!!! :o)
I started making changes in April by learning to carb count and work out insulin ratios according to the amount of carbs I am going to eat so the next step is to apply what I have learnt to the insulin pump. I'm a bit nervous about managing to work out basal rates etc. but that will all be done with the help of my DSN on Monday and there will be plenty of ongoing support for me from her in the weeks and months to come.
Below are a few advantages and disadvantages of insulin pumps which must be considered before making a decision about whether a pump is right for you:
(Taken from http://www.input.me.uk/)
Disadvantages
•Being attached to the pump almost all of the time (the pump can instantly be disconnected for brief periods " swimming, showers, sex, etc.)
•Risk of diabetic Ketoacidosis (DKA) may be higher without frequent blood glucose testing
•Chance of skin infections, especially if the infusion set is not changed after 3 days
Advantages
•Offers a better quality of life and well being
•Freedom from a fixed insulin dose schedule
•Eat what you choose, when you like
•Ajust insulin to meet the body"s needs
•Feeling "normal"
•Being more alert & aware
•Being in control of life as well as diabetes
•Convenience
•Easier management of exercise, sport
•Reliable insulin action
•Staying up late, having a lie-in, or oversleeping without worry
•Restoration of hypoglycaemia awareness
•Managing the dawn phenomenon
•Travelling across time zones without missing or taking too much insulin
•Tight diabetes control before and during pregnancy
•Delay or prevention of long term complications
As you can see the advantages outnumber the disadvantage by far.....
Starting on the pump is going to be a massive life change, one which I am finally ready to accept. It's almost like throwing out everything I have ever known about Diabetes and starting all over again at the bottom of a pretty steep learning curve. I am so lucky to have been given the chance to make my way up to the top of the curve.
For years and years I just did the same doses with every meal, no matter what I was eating, no matter what exercise I did (if any) and I just did this without thinking about any of it. Starting with carb counting and going onto the pump has made me realise that it's not as straight forward as that if you want to take proper care of yourself. The next few months are going to be a lot of hard work in terms of more blood sugar testing, recording everything I eat and everything I do to see whether the basal rates are correct. I am totally ready to do everything I need to do to stay on the path of good Diabetic control for the first time ever!!!
As Monday gets closer I do have mixed emotions about getting "connected".....one minute I am high as a kite with excitement then I get a sudden surge of slight panic. Then I think about the people I've got around me and I know that with their help and support I will be just fine and will soon get used to having my pump and, before I know it it will be as though it has always been a part of me........
I'm sure some people won't understand how I can be feeling anything but excitement about getting my pump, especially people who have had or are having a fight on their hands to get one. I certainly don't want to annoy anyone by sounding ungrateful because that is not the case at all, I am extremely grateful for the opportunity I have been given and always will be.
It's hard to explain my feelings about Monday.....
I guess the word would be "apprehension". There are a few things I feel a bit nervous about, one being the fact that I will be more or less permanently attached to something for the rest of my life....ok, so I got on fine with it during my 3 day trial at the weekend and I do know that you can disconnect for short periods of time, but I do feel a bit freaked out by the "alien" element of it all. I have done a bit of reading on accepting being attached to the pump in my new "bible" (Pumping Insulin by John Walsh and Ruth Roberts). It mentions that some people may feel embarassed or self conscious about wearing a pump. I have to say that I am not concerned about that at all, in fact I am quite looking forward to telling people about it and explaining what it is and how it works, as it is certainly nothing to be ashamed of and I think the more people that know what it is and understand something about how it works the better. It's not how it looks to other people that concerns me, I think for me it's the "attachment" element of it which is quite hard to put into words. If anyone else had similar thoughts before starting on their pump please let me know.....(then again it might just be me!!! Lol)
Again, I do want to make it really clear that overall I am VERY happy about getting my pump and these negatives I'm talking about today are only small niggles, not major concerns!!!! I think it would be difficult to do something so life changing without feeling some sort of nervousness or anxiety.
I have been doing injections for 19 years now (first with a syringe and a glass vial of insulin that you had to draw up into the syringe yourself then with pens with cartridges that you changed and then finally with disposable, pre-filled pens) so I think I am going to find it really strange at first when I no longer have to reach for the insulin pen at set times of the day and for a while I might have to get Gareth to hide my pens so I don't inject!!! :o)
I started making changes in April by learning to carb count and work out insulin ratios according to the amount of carbs I am going to eat so the next step is to apply what I have learnt to the insulin pump. I'm a bit nervous about managing to work out basal rates etc. but that will all be done with the help of my DSN on Monday and there will be plenty of ongoing support for me from her in the weeks and months to come.
Below are a few advantages and disadvantages of insulin pumps which must be considered before making a decision about whether a pump is right for you:
(Taken from http://www.input.me.uk/)
Disadvantages
•Being attached to the pump almost all of the time (the pump can instantly be disconnected for brief periods " swimming, showers, sex, etc.)
•Risk of diabetic Ketoacidosis (DKA) may be higher without frequent blood glucose testing
•Chance of skin infections, especially if the infusion set is not changed after 3 days
Advantages
•Offers a better quality of life and well being
•Freedom from a fixed insulin dose schedule
•Eat what you choose, when you like
•Ajust insulin to meet the body"s needs
•Feeling "normal"
•Being more alert & aware
•Being in control of life as well as diabetes
•Convenience
•Easier management of exercise, sport
•Reliable insulin action
•Staying up late, having a lie-in, or oversleeping without worry
•Restoration of hypoglycaemia awareness
•Managing the dawn phenomenon
•Travelling across time zones without missing or taking too much insulin
•Tight diabetes control before and during pregnancy
•Delay or prevention of long term complications
As you can see the advantages outnumber the disadvantage by far.....
Starting on the pump is going to be a massive life change, one which I am finally ready to accept. It's almost like throwing out everything I have ever known about Diabetes and starting all over again at the bottom of a pretty steep learning curve. I am so lucky to have been given the chance to make my way up to the top of the curve.
For years and years I just did the same doses with every meal, no matter what I was eating, no matter what exercise I did (if any) and I just did this without thinking about any of it. Starting with carb counting and going onto the pump has made me realise that it's not as straight forward as that if you want to take proper care of yourself. The next few months are going to be a lot of hard work in terms of more blood sugar testing, recording everything I eat and everything I do to see whether the basal rates are correct. I am totally ready to do everything I need to do to stay on the path of good Diabetic control for the first time ever!!!
As Monday gets closer I do have mixed emotions about getting "connected".....one minute I am high as a kite with excitement then I get a sudden surge of slight panic. Then I think about the people I've got around me and I know that with their help and support I will be just fine and will soon get used to having my pump and, before I know it it will be as though it has always been a part of me........
Monday, 2 August 2010
What a Week It's Been!!!
Well, it's been a busy old week in terms of my Diabetes....
Last Wednesday was another session of laser treatment for Diabetic Retinopathy (which I did a huuuuuuge blog post on last week). As usual, even though I have had quite a few sessions on both eyes in the last few years, I was terrified and got myself in a right old state beforehand.
Ever since the first time I had it done and I fainted I have had to have the anaesthetic injection in my eye before the laser session so I was quite prepared to have it done again, in fact, although it's not very nice and it involves them making a small cut in your eye ball, I would much rather have that than have to feel the pain / weird sensation that you get when your being lasered and risk fainting again so that they can't carry on and finish the session. Anyway, the doctor, who I had never seen before (I hate they way it is a different doctor that does it every single time!!!) decided that she didn't want to give me the injection. She said: "a lot of people tell me I'm very gentle with the laser" which didn't really make me feel any better but even though I said I really would prefer to have the injection she insisted that we would just "see how it went without it".....I was not happy at all and I started to panic even more. To do the laser burns they have to shine an incredibly bright white light into your eye which always makes my other eye instinctively close, which then makes the eyeball that they are trying to laser move around....the doctor told me to try and keep my left eye open so that my right eye wouldn't move so I tried to explain to her that this is one of the reasons I always have the injection first so that it numbs my eye and it won't move during the lasering but all she said was "oh well".....Great!!
It didn't hurt too much for the first few burns but after about 5 minutes it got really sore and I started to feel faint and queasy so we had to stop....this happened another 2 times, by which point I was in a lot of pain (which can happen when you have had a lot of previous sessions) and felt very hot and sweaty and the room was spinning. At this point she decided to stop. I really did feel as though she hadn't done enough but knew that for her to carry on she would have to do the injection as I was in a lot of pain and she just did not want to do it. I got the impression from the minute I walked in the room that she just couldn't be bothered doing the anaesthetic procedure for me. I'm sure plenty of people can easily take the pain and discomfort of having it done but everyone is different and has a different pain threshold so I'm really not happy that she just fobbed me off and made me feel as though I was being pathetic!!!! Before she sent me off home she said "I've made a note that for your next appointment you do need the anaesthetic doing first"......I do hate to say I told you so but.......
Next time (31st August for my left eye) I am going to refuse to have it done unless they agree to give me the anaesthetic injection first and I do not want to see that same doctor again for laser treatment.
The next day was not nearly as horrible......it was my appointment at Stafford Hospital to start my insulin pump trial....how exciting!!! I was expecting to take 2 home for the weekend but when we got there we discussed the 2 types and decided that I would only take home the Medtronic pump. We discussed how I had been getting on with the carb counting and how I had been feeling in general. I have been having far less headaches than I used to, I am able to stay awake much later than I used to - I used to get in from work and could easily fall straight to sleep or go to bed at 8.00 pm because I was constantly exhausted and I have been having quite a few more hypos than I used to. Before I went on holiday I had my HbA1c done and amazingly it had come down from 11.6 in March to.....wait for it......8.8!!!!!!! (For those not in the know already, the target they always tell you to aim for is 6.5 so I am getting there). I am so pleased that it has come down by that much already. I did expect it to have come down but not by that much (it might not sound like much but in terms of HbA1c results every 1% counts a hell of a lot). This reduction would explain why I have been feeling less tired and been having less headaches. See below for a description of what the HbA1c test actually is........
HbA1c Tests
The HbA1c test, indicates your blood glucose levels for the previous two to three months. HbA1c (glycosylated haemoglobin) is a measure of the amount of glucose attached to the body’s red blood cells; it is present in everyone. The level of HbA1c in your body rises and falls in line with your blood glucose – the higher your HbA1c, the more glucose is attached to your red blood cells.
Your HbA1c does not change rapidly because the red blood cells in your circulation last for around 3–4 months. Any increases and decreases in your HbA1c will happen over a period of at least 6 weeks. An HbA1c test is not the same as a blood glucose test. Your HbA1c test may be done using a blood sample taken from your arm or from a finger prick test.
HbA1c Targets
For most people with diabetes, the HbA1c target is below 6.5 per cent, since evidence shows that this can reduce the risk of developing diabetic complications, such as nerve damage, eye disease, kidney disease and heart disease.
Individuals at risk of severe hypoglycaemia should aim for an HbA1c of less than 7.5 per cent. However, any reduction in HbA1c levels (and therefore, any improvement in control), is still considered to have beneficial effects on the onset and progression of complications.
HbA1c Results
HbA1c results are currently given as a percentage. However, the way in which HbA1c results are reported in the UK is changing. From 31 May 2011, HbA1c will be given in millimoles per mol (mmol/mol) instead of as a percentage (%). To help make this transition as easy as possible, all HbA1c results in the UK will be given in both percentage and mmol/mol from 1 June 2009 until 31 May 2011.
This new way of reporting results will just be a different way of expressing the same thing. For example, the equivalent of the HbA1c target of 6.5 per cent will be 48 mmol/mol. The fact that the number is higher does not mean there is more glucose in your blood.
So anyway, back to the pump trial....I had a quick practice with an infusion set for the Medtronic pump and then once we had had a look through the menus on the pump screen I was given all the bits of kit I needed to take home with me for the weekend.....infusion set, saline, alcohol wipe, infusion set inserter, the pump, reservoir for the insulin (saline for the trial) and off I went.
We decided to go to my Mom's to set up the pump and put in the infusion set so I could show her how it works (I was dying to show off my new "toy"). I had a bit of a 'faff' with drawing up the saline into the reservoir but after that it was all plain sailing and I did my very first insertion all on my own. I was really surprised just how painless it was and then during the evening I was surprised that I managed to forget it was even there!!!!
Spending our first night sharing our bed with the pump was fine apart from me rolling on it a few times as the one I had on loan did not have a waistband clip on the back and I couldn't attach it to my PJ's.
On Friday I loved showing off the pump to people in my office and explaining all about it which has earned me the new nickname of "the bionic woman".
I had a bit of a play around with the menus over the weekend and gave myself "fake" doses of saline but that part of it (setting the basal rates etc. etc.) will be explained to me at the training on 9th August.
The only two minor "freak outs" I had were when I was in the shower and the pump was disconnected from the infusion set.....I knocked the infusion set a couple of times and for some reason that really made it hit home that I will have one of them in my stomach forever from now on. For some weird reason I found it stranger to look at it when the pump was disconnected from the infusion set/my stomach and all that was left was the device lodged in my stomach...I'm not sure why this made me feel so strange but I guess it's just all part of getting used to this new "part of me" and my new way of life.
When I took the pump off on Sunday morning I immediately felt "lost" without it which I think must be a good sign as I must admit the part I had been mot worried about was getting used to being attached to something "alien" for the rest of my life so if I already feel lost without it that can only be a good indication that I will soon get used to that side of it all.
All in all the trial went really well, much smoother that I expected, and I am now really excited to get started on my own pump and start to learn all of the more 'technical' aspects of using the pump. The trial was more about getting an idea of how it will feel to actually wear the pump.
Today I contacted my DSN at the hospital to let her know that it went well and that I would like her to go ahead and order my (bubblegum pink) pump from Medtronic!!!!
http://www.medtronic-diabetes.co.uk/product-information/paradigm-veo/index.html
I can't believe that this time next week I will be "connected" and I will be a member of the "insulin pumping community". I am so grateful for all the help I have had from my DSN's at my GP's in getting me referred, from my dietician at the hospital, from my new consultant and from my new DSN at the hospital. It has been a very short "journey" from injections to pump and I really do appreciate how lucky I am to have even got funding for a pump, let alone get one so quickly.
All that's left for me to do now is think of a name for my new pump :o)
ROLL ON MONDAY 9TH AUGUST!!!!!!!
Last Wednesday was another session of laser treatment for Diabetic Retinopathy (which I did a huuuuuuge blog post on last week). As usual, even though I have had quite a few sessions on both eyes in the last few years, I was terrified and got myself in a right old state beforehand.
Ever since the first time I had it done and I fainted I have had to have the anaesthetic injection in my eye before the laser session so I was quite prepared to have it done again, in fact, although it's not very nice and it involves them making a small cut in your eye ball, I would much rather have that than have to feel the pain / weird sensation that you get when your being lasered and risk fainting again so that they can't carry on and finish the session. Anyway, the doctor, who I had never seen before (I hate they way it is a different doctor that does it every single time!!!) decided that she didn't want to give me the injection. She said: "a lot of people tell me I'm very gentle with the laser" which didn't really make me feel any better but even though I said I really would prefer to have the injection she insisted that we would just "see how it went without it".....I was not happy at all and I started to panic even more. To do the laser burns they have to shine an incredibly bright white light into your eye which always makes my other eye instinctively close, which then makes the eyeball that they are trying to laser move around....the doctor told me to try and keep my left eye open so that my right eye wouldn't move so I tried to explain to her that this is one of the reasons I always have the injection first so that it numbs my eye and it won't move during the lasering but all she said was "oh well".....Great!!
It didn't hurt too much for the first few burns but after about 5 minutes it got really sore and I started to feel faint and queasy so we had to stop....this happened another 2 times, by which point I was in a lot of pain (which can happen when you have had a lot of previous sessions) and felt very hot and sweaty and the room was spinning. At this point she decided to stop. I really did feel as though she hadn't done enough but knew that for her to carry on she would have to do the injection as I was in a lot of pain and she just did not want to do it. I got the impression from the minute I walked in the room that she just couldn't be bothered doing the anaesthetic procedure for me. I'm sure plenty of people can easily take the pain and discomfort of having it done but everyone is different and has a different pain threshold so I'm really not happy that she just fobbed me off and made me feel as though I was being pathetic!!!! Before she sent me off home she said "I've made a note that for your next appointment you do need the anaesthetic doing first"......I do hate to say I told you so but.......
Next time (31st August for my left eye) I am going to refuse to have it done unless they agree to give me the anaesthetic injection first and I do not want to see that same doctor again for laser treatment.
The next day was not nearly as horrible......it was my appointment at Stafford Hospital to start my insulin pump trial....how exciting!!! I was expecting to take 2 home for the weekend but when we got there we discussed the 2 types and decided that I would only take home the Medtronic pump. We discussed how I had been getting on with the carb counting and how I had been feeling in general. I have been having far less headaches than I used to, I am able to stay awake much later than I used to - I used to get in from work and could easily fall straight to sleep or go to bed at 8.00 pm because I was constantly exhausted and I have been having quite a few more hypos than I used to. Before I went on holiday I had my HbA1c done and amazingly it had come down from 11.6 in March to.....wait for it......8.8!!!!!!! (For those not in the know already, the target they always tell you to aim for is 6.5 so I am getting there). I am so pleased that it has come down by that much already. I did expect it to have come down but not by that much (it might not sound like much but in terms of HbA1c results every 1% counts a hell of a lot). This reduction would explain why I have been feeling less tired and been having less headaches. See below for a description of what the HbA1c test actually is........
HbA1c Tests
The HbA1c test, indicates your blood glucose levels for the previous two to three months. HbA1c (glycosylated haemoglobin) is a measure of the amount of glucose attached to the body’s red blood cells; it is present in everyone. The level of HbA1c in your body rises and falls in line with your blood glucose – the higher your HbA1c, the more glucose is attached to your red blood cells.
Your HbA1c does not change rapidly because the red blood cells in your circulation last for around 3–4 months. Any increases and decreases in your HbA1c will happen over a period of at least 6 weeks. An HbA1c test is not the same as a blood glucose test. Your HbA1c test may be done using a blood sample taken from your arm or from a finger prick test.
HbA1c Targets
For most people with diabetes, the HbA1c target is below 6.5 per cent, since evidence shows that this can reduce the risk of developing diabetic complications, such as nerve damage, eye disease, kidney disease and heart disease.
Individuals at risk of severe hypoglycaemia should aim for an HbA1c of less than 7.5 per cent. However, any reduction in HbA1c levels (and therefore, any improvement in control), is still considered to have beneficial effects on the onset and progression of complications.
HbA1c Results
HbA1c results are currently given as a percentage. However, the way in which HbA1c results are reported in the UK is changing. From 31 May 2011, HbA1c will be given in millimoles per mol (mmol/mol) instead of as a percentage (%). To help make this transition as easy as possible, all HbA1c results in the UK will be given in both percentage and mmol/mol from 1 June 2009 until 31 May 2011.
This new way of reporting results will just be a different way of expressing the same thing. For example, the equivalent of the HbA1c target of 6.5 per cent will be 48 mmol/mol. The fact that the number is higher does not mean there is more glucose in your blood.
So anyway, back to the pump trial....I had a quick practice with an infusion set for the Medtronic pump and then once we had had a look through the menus on the pump screen I was given all the bits of kit I needed to take home with me for the weekend.....infusion set, saline, alcohol wipe, infusion set inserter, the pump, reservoir for the insulin (saline for the trial) and off I went.
We decided to go to my Mom's to set up the pump and put in the infusion set so I could show her how it works (I was dying to show off my new "toy"). I had a bit of a 'faff' with drawing up the saline into the reservoir but after that it was all plain sailing and I did my very first insertion all on my own. I was really surprised just how painless it was and then during the evening I was surprised that I managed to forget it was even there!!!!
Spending our first night sharing our bed with the pump was fine apart from me rolling on it a few times as the one I had on loan did not have a waistband clip on the back and I couldn't attach it to my PJ's.
On Friday I loved showing off the pump to people in my office and explaining all about it which has earned me the new nickname of "the bionic woman".
I had a bit of a play around with the menus over the weekend and gave myself "fake" doses of saline but that part of it (setting the basal rates etc. etc.) will be explained to me at the training on 9th August.
The only two minor "freak outs" I had were when I was in the shower and the pump was disconnected from the infusion set.....I knocked the infusion set a couple of times and for some reason that really made it hit home that I will have one of them in my stomach forever from now on. For some weird reason I found it stranger to look at it when the pump was disconnected from the infusion set/my stomach and all that was left was the device lodged in my stomach...I'm not sure why this made me feel so strange but I guess it's just all part of getting used to this new "part of me" and my new way of life.
When I took the pump off on Sunday morning I immediately felt "lost" without it which I think must be a good sign as I must admit the part I had been mot worried about was getting used to being attached to something "alien" for the rest of my life so if I already feel lost without it that can only be a good indication that I will soon get used to that side of it all.
All in all the trial went really well, much smoother that I expected, and I am now really excited to get started on my own pump and start to learn all of the more 'technical' aspects of using the pump. The trial was more about getting an idea of how it will feel to actually wear the pump.
Today I contacted my DSN at the hospital to let her know that it went well and that I would like her to go ahead and order my (bubblegum pink) pump from Medtronic!!!!
http://www.medtronic-diabetes.co.uk/product-information/paradigm-veo/index.html
I can't believe that this time next week I will be "connected" and I will be a member of the "insulin pumping community". I am so grateful for all the help I have had from my DSN's at my GP's in getting me referred, from my dietician at the hospital, from my new consultant and from my new DSN at the hospital. It has been a very short "journey" from injections to pump and I really do appreciate how lucky I am to have even got funding for a pump, let alone get one so quickly.
All that's left for me to do now is think of a name for my new pump :o)
ROLL ON MONDAY 9TH AUGUST!!!!!!!
Labels:
HbA1c,
medtronic,
retinopathy
Thursday, 29 July 2010
Pump Practice!!!!
Just a short post today....but sometimes less is more!!!!! ;o)
The picture is me "modelling" the 'Medtronic MiniMed Paradigm Veo' insulin pump. I am having a "play" with it over the weekend and will be getting my own on the 9TH AUGUST!!!!!!! 11 DAYS TO GO!!!!!!!!!!!!!!!!!!!
Pretty much all I can say about it for now is "AAAAGGGHHHHHHH" because I AM SO EXCITED & HAPPY. I was really quite nervous before my appointment today in terms of there being a hell of a lot to take in but I think that part of it is going to be on the start day when I get the full training. Today was more just about putting an infusion set in and then I can have a play with all the menus and features on the pump over the weekend. I was pretty nervous about doing the first set insert but I had one go at doing one without it being attached to the pump, while I was still at the hospital then I did it all, including filling the reservoir with saline and priming the tubing etc. without having been shown how to do it by the DSN, on my own when I got home so I'm pretty pleased with how easily I managed to do it all especially as the DSN hadn't shown me how to do those parts of it at the appointment. The set insert was nothing to worry about, I hardly felt it go in and now as I'm sitting here typing away, I can't feel it at all.....
So far, I love it...I've got to spend the... weekend having a look at all the menus and features then my DSN is going to get my own pink one ordered for me on Monday!!!!!
Oh, and some more great news today.....my last HbA1c was 11.6 (in March) and today I found out it has come down to 8.8 so I'm really pleased and also pleasantly surprised as I had expected it to have come down but not by that much!!!! All the hard work and carb counting is certainly paying off!!!!
Obviously the hard work with the pump is really going to begin on the start day but I'm more than ready for it and can't wait to get started for real.....
Off to have a lie down now so I can recover from all the excitement....(God knows what I'm going to be like on 9th August)
P.S. I am of course going to have to give my new pink pump a name so if anyone has any suggestions please let me know..... :o)
Monday, 26 July 2010
Diabetic Retinopathy - The Facts
Apologies in advance for the length of this post!!!! Today's post is going to be totally factual rather than me just rambling on about what I've been up to and it will hopefully explain everything you need to know about Diabetic Retinopathy, including how it occurs, symptoms, the NHS National Screening Programme, how it affects the eye(s), the different stages of the disease, the treatment involved, how to help to prevent the disease and the outlook for people who have Retinopathy.
I realise I have done part of a blog about this before but I really want to try and raise awareness of this particular complication of Diabetes as it's very close to my heart, so I'm sure you won't mind me repeating myself a bit!!! Oh, and by the way, I have to admit that a lot of the factual information is taken from various websites and not actually written 100% by me, as you will probably be able to tell.
WHAT IS DIABETIC RETINOPATHY???
Retinopathy is a general term used to describe various disorders of the retina. Retinopathy is caused by the tiny blood vessels next to the retina and is often a result of diabetes, hence the term 'diabetic retinopathy.'
WHAT IS THE OUTLOOK FOR PEOPLE WITH DIABETIC RETINOPATHY???
Diabetes can have a number of effects on our vision. The most common is on the retina. The walls of the blood vessels in our eyes can become weak and over time, the walls begin to bulge. This creates an 'eddy' in the blood flow which can eventually block. Blood and other fluids start to leak into the retina and hard deposits are left there. Because of the reduction in blood flow the body grows new blood vessels. However, these veins are fragile and tend to rupture suddenly leaking blood into the vitreous. This will lead to a sudden and dramatic loss of vision, however, this may clear over time.
HOW THE EYE WORKS
Your eye has a lens and an aperture (opening) at the front known as the pupil, which adjust to bring objects into focus on the retina at the back of the eye. The retina is made up of a delicate tissue that is sensitive to light, rather like the film in a camera. It also contains a fine network of small blood vessels.
At the centre of the retina is the macula, which is a small area about the size of a pinhead. This is the most highly specialised part of the retina and is vital because it allows you to see fine detail for activities such as reading and writing and also to recognise colours. The other parts of the retina give you side vision (peripheral vision). Filling the space in front of the retina is a clear jelly-like substance called the vitreous gel.
THE NHS NATIONAL SCREENING PROGRAMME
In 2005 The Department of Health set up a national screening programme for diabetic retinopathy. If you are 11 years of age or over and you have diabetes, you should be offered annual screening. The screening programme was introduced because, if diabetic retinopathy is detected early enough, it can be treated effectively using laser treatment.
During screening, eye drops are used to make your pupils large and photographs of your retina are taken. As the photographs are being taken, you will see flashes of bright light, but usually it is not uncomfortable. The eye drops may cause your eyes to sting slightly and your vision may become blurred about 15 minutes after the procedure ends. The blurring can last between two and six hours, depending on what sort of eye drops were used.
SYMPTOMS OF DIABETIC RETINOPATHY
Diabetic retinopathy does not usually cause any symptoms until it has reached an advanced stage. In some cases, the only noticeable symptom is a sudden and complete loss of vision. This is why regular screening is so important.
Symptoms of diabetic retinopathy include:
•discoloured spots (known as floaters that ‘float’ in your field of vision
•blurred vision
•your vision becomes blocked by patches or streaks
•reduced night vision, and, most serious
•sudden vision loss
RISK FACTORS FOR DIABETIC RETINOPATHY
Duration of Diabetes
The biggest risk factor for diabetic retinopathy is the length of time that you have lived with diabetes. For people with type 1 diabetes, 90% will have some degree of diabetic retinopathy after 10 years of having symptoms. For people with type 2 diabetes who do not need to take insulin, 67% will have some degree of diabetic retinopathy after 10 years of symptoms. For people with type 2 diabetes who need to take insulin, 79% will have some degree of diabetic retinopathy after 10 years of symptoms.
Blood Glucose Level
The higher the levels of glucose in your blood, the greater your risk of developing diabetic retinopathy. People with high blood glucose levels are more likely to progress to advanced diabetic retinopathy. Blood glucose levels are measured using a test known as the HbA1c test. HbA1c is a form of haemoglobin, the oxygen-carrying chemical in red blood cells that has glucose attached to it. Small changes in the levels of HbA1c can greatly affect the risk of developing diabetic retinopathy. For example, people with an HbA1c level of 8% are 40% more likely to develop diabetic retinopathy than people with an HbA1c level of 7%.
High Blood Pressure
People with high blood pressure (hypertension) are likely to progress to advanced diabetic retinopathy.
THE DIFFERENT STAGES OF DIABETIC RETINOPATHY
If diabetic retinopathy is detected during screening, you will be given information about how far the condition has progressed. This will determine the type of treatment you will receive.
Background Retinopathy
This is the first stage of diabetic retinopathy, it begins initially by acute swelling in the walls of the blood vessels. Spots known as micro aneurysms form on the retina and appear on the wall as small red coloured dots. There are also small yellow patches, which may form. This is a result of exuding protein from the blood stream onto the retina. Other marks on the retina at this stage could potentially be a haemorrhage, which appears in a similar form. At this stage of retinopathy, it will not directly affect your vision, however, regular checks are advised to keep the condition well monitored.
Pre-proliferative Retinopathy
This is the second stage. By this stage, new blood vessels have started to form in the retina and there are multiple points of bleeding.
Maculopathy
By this time, the macula (the most sensitive part of the retina) has been damaged.
Maculopathy, which leads to the sight threatening condition macula oedema, is when the blood vessels become more delicate and begin to leak. In the early stages, fluid from this can leak into the macula, which operates our immediate, straight-ahead vision, resulting in swelling and blurred vision. The macula is an extremely sensitive area of the retina and macula oedema is one of the most common causes of visual impairment that you can develop through diabetes.
During the maculopathy stage, the haemorrhage's, swellings and leakages of protein as seen in the background retinopathy stage all begin to affect the macula. Specifically, this affects our ability to see finer details, for example, fine print in books.
These leakages can be cured by laser eye treatment, but often, several years later, more is needed to ensure they are properly treated. The leaks are known as clinically significant macula oedema and it takes four to six weeks for the treatment to take any sort of effect. As the condition develops, if left untreated it could become very severe. Should severe maculopathy occur, it will be very difficult to treat.
Proliferative Retinopathy
This is the most advanced stage. Proliferative retinopathy begins by the blood vessels within the retina becoming blocked. As a result of the insufficient blood flow to the retina, new, abnormally sized blood vessels begin to grow. Because these new blood vessels are very delicate and fragile, as they grow they are easily broken and can leak or bleed. The vessels are so easily broken that even sudden head movements such as sneezing, or rapid eye movement during sleep can cause them to break. They leak into the vitreous, causing a vitreous haemorrhage. The vitreous is a jelly like substance, which fills the centre of the eye to support its structure and give it its shape. As these vessels grow, they stimulate the growth of further abnormal tissue and as they break, they will eventually cause scar tissue to form. As a result of this, eventually the retina will detach itself altogether from the back of the eye.
TREATMENTS
Laser Treatment
The type of laser treatment used to treat diabetic retinopathy is known as photocoagulation. Photocoagulation involves using a laser to burn away any abnormal blood vessels.
A course of photocoagulation involves one or more visits to a laser treatment clinic. Treatment is normally available on an out-patient basis. It is not usually painful, but you may feel an occasional sharp pricking sensation when certain areas of your retina are being treated.
Drops are put into your eyes to numb the surface but you may still find the procedure slightly uncomfortable. A special contact lens is then placed on your eye to hold your lids open and to focus the laser beam on your retina.
As time goes on and more laser sessions are needed, the treatment can become extremely painful. There is no entirely effective way of reducing all the pain, except a general anaesthetic.
Local anaesthetic injections in the operating theatre, or tablets that aid relaxation, may help a little. Sometimes the local anaesthetic injection takes away all the pain, sometimes it just reduces the pain slightly. The injection is not into the eye, but under it, at one side. This type of anesthesia may be used when an extensive amount of laser is required, the patient has difficulty keeping the eye still, or the patient is very sensitive.
For patients where the treatment is extremely painful larger departments offer general anaesthetics, as these also have the advantage of allowing laser treatment to both eyes. To do this the department must have a laser that can be used in an operating theatre.
Your vision will be blurred after treatment, but this should return to normal after a few hours. If you have a lot of treatment on your eyes, it can cause them to ache. Over-the-counter (OTC) painkillers, such as paracetamol, should help ease the pain.
A 30 year old person with a lot of new vessels may need 6000 laser burns per eye, or even more, to prevent the new vessels growing. Other people usually need less. In patients with very severe disease so much laser may be required that the side vision becomes poor and driving unsafe: the aim of the treatment is to keep good central sight, that is sight looking straight ahead, which is need to read, work, and watch television.
Sometimes, photocoagulation can damage the outer retina. If this occurs, there is a chance that your night and peripheral vision (your ability to see to objects that are outside your direct gaze) may be affected. More than 50% of people who have laser treatment for diabetic retinopathy notice some difficulty with their night vision, and 3% notice some loss of peripheral vision.
Vitreous Surgery
This is often required if:
•a large amount of blood has collected in the centre of the eye, obscuring your vision, or
•there is extensive scar tissue which is likely to cause, or has already caused, retinal detachment
The surgeon will make a small incision in your eye before removing the vitreous gel that sits in front of the retina. The vitreous gel is where the blood gathers.
Any scar tissue will be removed from your retina and, in some cases, the retina may be strengthened in position using tiny clamps. The vitreous gel will be replaced with a gas or liquid to help hold the retina in place. The gas or liquid will gradually be absorbed by your body, which will create new gel to replace the gel that was removed during surgery.
Vitreous surgery is usually performed under local anaesthetic and sedation. This means that you will feel no pain and have little or no awareness of the surgery being performed. You should be able to go home on the same day or the day after your surgery.
For the first few days after surgery, you may be asked to wear an eye patch so that you can gradually make more and more use of your eye. This is because activities such as reading and watching television can quickly tire your eye.
Following vitreous surgery, it is normal to have blurred vision for several weeks. This should begin to improve gradually, though it may take several months before your vision returns to normal.
PREVENTION
To prevent or slow the progression of diabetic retinopathy, it is very important to keep your blood sugar level as close to normal as possible.
Having high blood pressure (hypertension) can make the blood vessels in your eyes more vulnerable to damage, increasing your risk of developing advanced diabetic retinopathy. The most effective way of preventing high blood pressure is to eat a healthy, balanced diet, including plenty of fruit and vegetables (at least five portions a day), and to take regular exercise (at least 30 minutes five times a week).
If diabetic retinopathy is diagnosed and treated at an early stage, the outlook for the condition is good. Research has found that treatment can prevent severe vision loss in 90% of cases of diabetic retinopathy.
I hope (if you are still awake after reading all of that) that the post has answered a few questions about what Retinopathy is and what is involved in the treatment available.
Some useful websites are:
http://medweb.bham.ac.uk/easdec/Information_for_patients.html
http://www.nhs.uk/Conditions/Diabetic-retinopathy/Pages/Introduction.aspx
http://www.youreyeguide.co.uk/retinopathy/index.html
Saturday, 24 July 2010
Riding the Roller Coaster
I think a good way to describe Diabetes is that it is like a roller coaster....there are ups and downs and lots of unexpected twists and turns along the way. These ups and downs and twists and turns can come in the form of the highs and lows of blood sugars and the sometimes unexpected diagnosis of a long term complication or maybe a request for a pump being turned down but they can also be related to the emotional side of living with Diabetes.
For me, an example of the emotions you can go through would be the last couple of days during which I have felt angry, hateful, tired, upset, tearful, self-pitying, irrational, like giving up, frustrated, powerless, pathetic, like a failure, guilty, energetic, motivated, happy, proud, relieved and disappointed....and that's just in the space of about 36 hours so imagine the range of emotions people with Diabetes go through from the date of diagnosis and then for the rest of your life.....that's a lot of ups and downs!!!
Yesterday was a bad day for me Diabetes-wise in terms of just wanting to ignore it and pretend it wasn't happening to me. During the day I felt anger and hatred towards this life long condition that has decided to inflict itself upon me and my family. I wanted it to go away and leave us all alone, even if it was just for a little while!!! Like I said yesterday, you sometimes feel like you want to ask Diabetes "why me?" and that was where the self-pitying came in. By the end of the day I felt like a total and utter failure and completely pathetic for not having the willpower to leave the chocolate alone and just do what I needed to do (i.e. count carbs, test sugars etc.).
Then as this morning came I felt guilty, like a fraud and like I had let everyone down. These feelings are because I have been extremely lucky in being given the chance to have an insulin pump and that means total commitment to it and to your Diabetes.....yesterday was not a good way to show my commitment or gratitude!!! My sugars first thing were 16.7 so I made the decision (a monumental one for a person such as me who can't stand exercise) to not get down about it and to do something positive so I dusted off one of my old dance workout dvd's and tried to reduce my sugar levels that way. It has been a looooong time since I did any exercise so afterwards I felt really good that I had done it and actually enjoyed it too. It's only a small step but every little helps, as they say.
Before lunch my sugar was down to 6.5 so the exercise had had a really positive effect on both my sugars and my mood (this was where the feelings of relief came in - I had totally changed my attitude from yesterday and done something good to improve my sugars - and it had worked). Then after lunch I suddenly felt hypo.....sugars down to 3.1.....aside from the shakiness, sweating, intense hunger and feeling weak there was the familiar feeling of disappointment!!!!! I thought I was doing so well in my attempt to be a "good Diabetic" today and then it all went wrong.
My sugars are currently 11.0 which isn't too bad (for me anyway) especially after treating a hypo earlier on. I'm back to feeling fairly positive and trying to focus on the fact that I'm getting my trial pumps next week so it's all becoming very real very quickly.....and of course, with that comes a whole new set of emotions.....
There really is no getting off this roller coaster that is Type 1 Diabetes!!!
P.S. Huge thank you to Gareth for putting up with all of these emotions and for riding the roller coaster with me!!! x x x
For me, an example of the emotions you can go through would be the last couple of days during which I have felt angry, hateful, tired, upset, tearful, self-pitying, irrational, like giving up, frustrated, powerless, pathetic, like a failure, guilty, energetic, motivated, happy, proud, relieved and disappointed....and that's just in the space of about 36 hours so imagine the range of emotions people with Diabetes go through from the date of diagnosis and then for the rest of your life.....that's a lot of ups and downs!!!
Yesterday was a bad day for me Diabetes-wise in terms of just wanting to ignore it and pretend it wasn't happening to me. During the day I felt anger and hatred towards this life long condition that has decided to inflict itself upon me and my family. I wanted it to go away and leave us all alone, even if it was just for a little while!!! Like I said yesterday, you sometimes feel like you want to ask Diabetes "why me?" and that was where the self-pitying came in. By the end of the day I felt like a total and utter failure and completely pathetic for not having the willpower to leave the chocolate alone and just do what I needed to do (i.e. count carbs, test sugars etc.).
Then as this morning came I felt guilty, like a fraud and like I had let everyone down. These feelings are because I have been extremely lucky in being given the chance to have an insulin pump and that means total commitment to it and to your Diabetes.....yesterday was not a good way to show my commitment or gratitude!!! My sugars first thing were 16.7 so I made the decision (a monumental one for a person such as me who can't stand exercise) to not get down about it and to do something positive so I dusted off one of my old dance workout dvd's and tried to reduce my sugar levels that way. It has been a looooong time since I did any exercise so afterwards I felt really good that I had done it and actually enjoyed it too. It's only a small step but every little helps, as they say.
Before lunch my sugar was down to 6.5 so the exercise had had a really positive effect on both my sugars and my mood (this was where the feelings of relief came in - I had totally changed my attitude from yesterday and done something good to improve my sugars - and it had worked). Then after lunch I suddenly felt hypo.....sugars down to 3.1.....aside from the shakiness, sweating, intense hunger and feeling weak there was the familiar feeling of disappointment!!!!! I thought I was doing so well in my attempt to be a "good Diabetic" today and then it all went wrong.
My sugars are currently 11.0 which isn't too bad (for me anyway) especially after treating a hypo earlier on. I'm back to feeling fairly positive and trying to focus on the fact that I'm getting my trial pumps next week so it's all becoming very real very quickly.....and of course, with that comes a whole new set of emotions.....
There really is no getting off this roller coaster that is Type 1 Diabetes!!!
P.S. Huge thank you to Gareth for putting up with all of these emotions and for riding the roller coaster with me!!! x x x
Friday, 23 July 2010
Damn You Diabetes!!!
I think the title of the post kind of says it all.....
Today I hate Diabetes.....
Today I have ignored Diabetes....
Today I pretended I was a non-Diabetic....
Today has been an "I can't be arsed with Diabetes" day. I used to spend my entire life having days like this where I ignored Diabetes completely but lately those kind of days have been non-existent.....until today!!!
I basically spent the day not counting carbs, eating absolute rubbish and not testing my sugars and now I feel like crap......Yes, it's all my own fault and yes, I've been a terrible Diabetic today but I have to say I enjoyed every minute of it and every piece of chocolate tasted great.......sometimes it feels good to stick 2 fingers up to this vile disease called Diabetes!!!!
As all of you with the dreaded D will know, there are times when you don't just dislike Diabetes but you HATE it and want to scream and shout "why me?" and if it was a physical thing you could grab hold of you would give it a good kicking and maybe a few punches too!!! (I'm not normally a violent person, honest.....but Diabetes really does bring out the worst in me sometimes!!)
There are times when you don't want to have to count how many carbs are in every single thing you eat, you don't want to weigh your food, you don't want to have to do the maths to calculate your insulin doses, you don't want to prick your finger and squeeze a drop of blood out of it every few hours, you don't give a s**t what your blood sugar level is and you just don't want to have Diabetes taking up any space in your head!!!!
But then you remember......it's not going to go away no matter how much you try and ignore it, it will still be there tomorrow, and the next day and the day after that.......
Oh well, tomorrow's another day and I can try and get back to being a "good diabetic" again.......
Today I hate Diabetes.....
Today I have ignored Diabetes....
Today I pretended I was a non-Diabetic....
Today has been an "I can't be arsed with Diabetes" day. I used to spend my entire life having days like this where I ignored Diabetes completely but lately those kind of days have been non-existent.....until today!!!
I basically spent the day not counting carbs, eating absolute rubbish and not testing my sugars and now I feel like crap......Yes, it's all my own fault and yes, I've been a terrible Diabetic today but I have to say I enjoyed every minute of it and every piece of chocolate tasted great.......sometimes it feels good to stick 2 fingers up to this vile disease called Diabetes!!!!
As all of you with the dreaded D will know, there are times when you don't just dislike Diabetes but you HATE it and want to scream and shout "why me?" and if it was a physical thing you could grab hold of you would give it a good kicking and maybe a few punches too!!! (I'm not normally a violent person, honest.....but Diabetes really does bring out the worst in me sometimes!!)
There are times when you don't want to have to count how many carbs are in every single thing you eat, you don't want to weigh your food, you don't want to have to do the maths to calculate your insulin doses, you don't want to prick your finger and squeeze a drop of blood out of it every few hours, you don't give a s**t what your blood sugar level is and you just don't want to have Diabetes taking up any space in your head!!!!
But then you remember......it's not going to go away no matter how much you try and ignore it, it will still be there tomorrow, and the next day and the day after that.......
Oh well, tomorrow's another day and I can try and get back to being a "good diabetic" again.......
Wednesday, 21 July 2010
Bits and Pieces......
Had a nice long break from Diabetes blogging and now it's about time I got back into it so here goes......
Not much to report really at the moment......had a great holiday in Turkey. We spent the entire 2 weeks doing virtually nothing which I'm sure sounds incredibly boring but it was exactly what we needed and we have come home fully rested, nicely tanned and a fair few pounds heavier....the all-inclusive constant eating regime was too good to resist I'm afraid. I would certainly recommend Turkey if you want fantastic weather, gorgeous scenery and friendly people and we really want to go back at some point.
On the Diabetes front the holiday went smoothly apart from the odd low which was easy to deal with with an extra ice cream or two and a couple of extreme highs, one of which was entirely my fault as on our last night I somehow managed to forget to inject with my evening meal....DOH!!!! At least I knew the reason for it though so I corrected and made sure I kept myself hydrated and everything was fine.
Before I went away on holiday I read about the JDRF's request for people to contact their local MP's to ask them to sign up to Early Day Motion (EDM) 122 regarding Type 1 Diabetes research, which Adrian Sanders MP had put down for the JDRF. Early Day Motions provide a formal mechanism for MPs to raise issues in the House of Commons. '
The full text of Early Day Motion 122 is below:
"That this House supports the Juvenile Diabetes Research Foundation (JDRF) in its campaign to increase awareness and understanding about type 1 diabetes; notes that type 1 and type 2 diabetes are very separate and distinct conditions; acknowledges that type 1 diabetes is a chronic, life-threatening auto immune condition and is not caused by eating sugary food, by being overweight or by lifestyle choices; further notes with concern that type 1 is a leading cause of kidney failure, adult blindness, stroke, heart attacks and nerve damage and that incidence of the condition is increasing by four per cent. year on year; further notes that approximately five per cent. of the entire NHS budget is spent on treating type 1 diabetes; recognises that JDRF is the world's leading charitable funder of type 1 diabetes research and the only organisation dedicated solely to finding the cure for type 1; and believes that more funding for medical research will lead to the development of better treatments for type 1 diabetes, resulting in fewer complications and hospitalisations, improve cost efficiencies for the NHS budget and lead to a cure."
I contacted my local MP for Wolverhampton North East, Emma Reynolds, by e-mail and have now had a letter back from her saying that she has signed up to the EDM, which I am really pleased about. At the time she replied a total of 36 MP's had signed up to it. If you would like to contact your local MP to ask them to sign up click on the JDRF website link below where you can find out more.
http://www.jdrf.org.uk/news.asp?section=23&itemid=1489
At my last appointment my DSN gave me one of the new Bayer Contour USB blood glucose meters to try, on condition that I do a review of it for her. I've been looking at the Contour USB for a while so to get one given to me for free was great. I have only started to use it this week so I haven't got much to say on it yet in terms of using the Glucofacts Software which allows you to view your meter readings and can produce a variety of reports but in terms of the look of it and how easy it is to use then I only have positive things to say. It looks really modern and funky and comes with multi coloured lancets which I quite like (Yes, I am very easily pleased I know!!!). When setting it up you can put in what your target results range is for before a meal and also for after a meal. Once you have put the drop of blood onto the test strip it asks you whether the test is before or after a meal and then when analysing the results it will tell you how many of your results have been on target or above or below the range you have set depending on whether the test was done before or after a meal. You can also add notes which you could use, for example, if you are ill and have a high result, you can add a note to the result so you have an explanation for it. You can also set reminders for when you want to do your next test. Once I have made use of the software and looked at the reports and graphs that can be produced I will do a proper review of it.
As I think I've mentioned before I have signed up to be a distributing volunteer for Diabetes UK and have just received my first box of materials. There are a few posters and a variety of leaflets. I can take some into work and will take some into my GP's and to the Eye Infirmary and Stafford Hospital next week. I will leave some at my local library also but I'm not sure where else to go with them if I'm honest. So if anyone has any ideas please let me know.....Thanks!!
Also before I went on holiday I e-mailed Diabetes UK about posting a link to my blog on their website. When I got home I still hadn't had a reply so I contacted them on their Facebook page and was told that they thought they had replied to me.....they hadn't so I sent my email again. The next day I had a response.......they aren't interested at this time as they already have someone blogging for them who is around my age and uses a pump. Bit disappointed if I'm totally honest but they have however, suggested that I can be a "guest blogger" at some point so watch this space......
Through an old school friend of mine I have got in contact with a girl in Canada who has been on a pump for 6 years. This is great as she has been able to tell me all about it and has re-iterated what I keep on hearing about how much the pump has changed her life.
Whilst I was on holiday I was contacted by a guy in America called John who had read my blog and liked the way I write so wanted my help with creating a new Facebook group called 'Diabetics with Neuropathy'. I'm not too sure at the moment exactly how I will be able to contribute as I do not have neuropathy myself but the group is now set up and with the help of Lee (Nevitt) I hope we can raise awareness of the condition and get the facts out there about this painful and debilitating complication of Diabetes.
I love making contact with new people who have Diabetes or have children with Diabetes as it means that this Diabetic Online Community of ours is just growing and growing and that can only be a good thing!!!
FINALLY I have some ketone test strips........after my unsuccessful trip to the GP's when the doctor had never even heard of ketones never mind strips that test for them, I got in touch with my wonderful DSN (Heidi) at the GP surgery and she got it all sorted out for me and put them onto my repeat prescription.
I've recently bought a couple of new Diabetes related books which I want to get started with really soon. One is called 'Pumping Insulin' by John Walsh and Ruth Roberts and the other is called '50 Diabetes Myths That Can Ruin Your Life and 50 Diabetes Truths That Can Save It' by Riva Greenberg.
The first one was recommended to me by a friend who has a pump and is apparently everything you need to know for success on an insulin pump. I have made a start reading it and so far it seems to be really informative and quite easy to follow. I think this one is going to be my "bible" over the next few months. I will do a proper review of it once I have read it all and maybe I can recommend it to other people who are soon to start with a pump.
I read an article on a website by the author of the second book and decided to buy her book. I haven't started it yet but I think it will be an interesting read. As I have said before, I'm currently trying to re-educate myself on all things Diabetes and learn about things to do with the disease that I have always ignored in the past so I think this book will be a good way of helping me to do that. Again, once I have read it I will do a quick review and let you know whether it's worth a look or not.....
A week today I will be going to the Eye Infirmary for more laser surgery on my right eye for my Retinopathy. Not looking forward to it one bit (obviously) but it's got to be done!!! I'm sure I will be able to get through it by thinking about my appointment the day after at Stafford Hospital with Gill, my DSN, to get 2 infusion sets put in so I can take 2 pumps home filled with saline to try them out and make my final decision on which one I want to have (I'm still thinking it's going to be the Medtronic - in pink of course - but I'll have to wait and see how I get on)......it's sooooo exciting and I can't wait!!!!!
Anyway, I think that's all the Diabetes related bits and pieces that have been going on recently.......thanks for reading!!! :o)
Not much to report really at the moment......had a great holiday in Turkey. We spent the entire 2 weeks doing virtually nothing which I'm sure sounds incredibly boring but it was exactly what we needed and we have come home fully rested, nicely tanned and a fair few pounds heavier....the all-inclusive constant eating regime was too good to resist I'm afraid. I would certainly recommend Turkey if you want fantastic weather, gorgeous scenery and friendly people and we really want to go back at some point.
On the Diabetes front the holiday went smoothly apart from the odd low which was easy to deal with with an extra ice cream or two and a couple of extreme highs, one of which was entirely my fault as on our last night I somehow managed to forget to inject with my evening meal....DOH!!!! At least I knew the reason for it though so I corrected and made sure I kept myself hydrated and everything was fine.
Before I went away on holiday I read about the JDRF's request for people to contact their local MP's to ask them to sign up to Early Day Motion (EDM) 122 regarding Type 1 Diabetes research, which Adrian Sanders MP had put down for the JDRF. Early Day Motions provide a formal mechanism for MPs to raise issues in the House of Commons. '
The full text of Early Day Motion 122 is below:
"That this House supports the Juvenile Diabetes Research Foundation (JDRF) in its campaign to increase awareness and understanding about type 1 diabetes; notes that type 1 and type 2 diabetes are very separate and distinct conditions; acknowledges that type 1 diabetes is a chronic, life-threatening auto immune condition and is not caused by eating sugary food, by being overweight or by lifestyle choices; further notes with concern that type 1 is a leading cause of kidney failure, adult blindness, stroke, heart attacks and nerve damage and that incidence of the condition is increasing by four per cent. year on year; further notes that approximately five per cent. of the entire NHS budget is spent on treating type 1 diabetes; recognises that JDRF is the world's leading charitable funder of type 1 diabetes research and the only organisation dedicated solely to finding the cure for type 1; and believes that more funding for medical research will lead to the development of better treatments for type 1 diabetes, resulting in fewer complications and hospitalisations, improve cost efficiencies for the NHS budget and lead to a cure."
I contacted my local MP for Wolverhampton North East, Emma Reynolds, by e-mail and have now had a letter back from her saying that she has signed up to the EDM, which I am really pleased about. At the time she replied a total of 36 MP's had signed up to it. If you would like to contact your local MP to ask them to sign up click on the JDRF website link below where you can find out more.
http://www.jdrf.org.uk/news.asp?section=23&itemid=1489
At my last appointment my DSN gave me one of the new Bayer Contour USB blood glucose meters to try, on condition that I do a review of it for her. I've been looking at the Contour USB for a while so to get one given to me for free was great. I have only started to use it this week so I haven't got much to say on it yet in terms of using the Glucofacts Software which allows you to view your meter readings and can produce a variety of reports but in terms of the look of it and how easy it is to use then I only have positive things to say. It looks really modern and funky and comes with multi coloured lancets which I quite like (Yes, I am very easily pleased I know!!!). When setting it up you can put in what your target results range is for before a meal and also for after a meal. Once you have put the drop of blood onto the test strip it asks you whether the test is before or after a meal and then when analysing the results it will tell you how many of your results have been on target or above or below the range you have set depending on whether the test was done before or after a meal. You can also add notes which you could use, for example, if you are ill and have a high result, you can add a note to the result so you have an explanation for it. You can also set reminders for when you want to do your next test. Once I have made use of the software and looked at the reports and graphs that can be produced I will do a proper review of it.
As I think I've mentioned before I have signed up to be a distributing volunteer for Diabetes UK and have just received my first box of materials. There are a few posters and a variety of leaflets. I can take some into work and will take some into my GP's and to the Eye Infirmary and Stafford Hospital next week. I will leave some at my local library also but I'm not sure where else to go with them if I'm honest. So if anyone has any ideas please let me know.....Thanks!!
Also before I went on holiday I e-mailed Diabetes UK about posting a link to my blog on their website. When I got home I still hadn't had a reply so I contacted them on their Facebook page and was told that they thought they had replied to me.....they hadn't so I sent my email again. The next day I had a response.......they aren't interested at this time as they already have someone blogging for them who is around my age and uses a pump. Bit disappointed if I'm totally honest but they have however, suggested that I can be a "guest blogger" at some point so watch this space......
Through an old school friend of mine I have got in contact with a girl in Canada who has been on a pump for 6 years. This is great as she has been able to tell me all about it and has re-iterated what I keep on hearing about how much the pump has changed her life.
Whilst I was on holiday I was contacted by a guy in America called John who had read my blog and liked the way I write so wanted my help with creating a new Facebook group called 'Diabetics with Neuropathy'. I'm not too sure at the moment exactly how I will be able to contribute as I do not have neuropathy myself but the group is now set up and with the help of Lee (Nevitt) I hope we can raise awareness of the condition and get the facts out there about this painful and debilitating complication of Diabetes.
I love making contact with new people who have Diabetes or have children with Diabetes as it means that this Diabetic Online Community of ours is just growing and growing and that can only be a good thing!!!
FINALLY I have some ketone test strips........after my unsuccessful trip to the GP's when the doctor had never even heard of ketones never mind strips that test for them, I got in touch with my wonderful DSN (Heidi) at the GP surgery and she got it all sorted out for me and put them onto my repeat prescription.
I've recently bought a couple of new Diabetes related books which I want to get started with really soon. One is called 'Pumping Insulin' by John Walsh and Ruth Roberts and the other is called '50 Diabetes Myths That Can Ruin Your Life and 50 Diabetes Truths That Can Save It' by Riva Greenberg.
The first one was recommended to me by a friend who has a pump and is apparently everything you need to know for success on an insulin pump. I have made a start reading it and so far it seems to be really informative and quite easy to follow. I think this one is going to be my "bible" over the next few months. I will do a proper review of it once I have read it all and maybe I can recommend it to other people who are soon to start with a pump.
I read an article on a website by the author of the second book and decided to buy her book. I haven't started it yet but I think it will be an interesting read. As I have said before, I'm currently trying to re-educate myself on all things Diabetes and learn about things to do with the disease that I have always ignored in the past so I think this book will be a good way of helping me to do that. Again, once I have read it I will do a quick review and let you know whether it's worth a look or not.....
A week today I will be going to the Eye Infirmary for more laser surgery on my right eye for my Retinopathy. Not looking forward to it one bit (obviously) but it's got to be done!!! I'm sure I will be able to get through it by thinking about my appointment the day after at Stafford Hospital with Gill, my DSN, to get 2 infusion sets put in so I can take 2 pumps home filled with saline to try them out and make my final decision on which one I want to have (I'm still thinking it's going to be the Medtronic - in pink of course - but I'll have to wait and see how I get on)......it's sooooo exciting and I can't wait!!!!!
Anyway, I think that's all the Diabetes related bits and pieces that have been going on recently.......thanks for reading!!! :o)
Subscribe to:
Posts (Atom)
Search This Blog
Labels
Diabetes UK
(1)
Diabetic Cheiroarthropathy
(1)
Facebook
(1)
Necrobiosis Lipoidica Diabeticorum
(1)
Support
(3)
basal
(2)
blood sugar
(1)
bolus
(2)
carbohydrate
(3)
carbs
(2)
cardiovascular disease
(1)
cravings
(2)
dietician
(2)
exercise
(1)
frustration
(2)
hyperglycemia
(1)
hypoglycemia
(2)
insulin
(4)
insulin pump
(1)
limited joint mobility
(1)
medication
(1)
pin cushion
(1)
sponsored walk
(1)

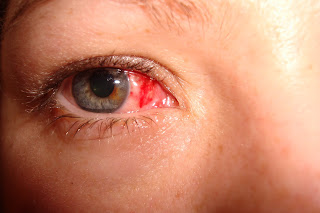







.JPG)



